Macular Degeneration (ARMD / AMD)
 Symptoms & Causes
Vitamins & Supplements
About the macula
Pathology
News
Symptoms & Causes
Vitamins & Supplements
About the macula
Pathology
News
The macula is responsible for our most highly focused vision: central vision. The macula is a small yellowish area at the center of the retina, it receives its yellow color from the pigmented antioxidants lutein, zeaxanthin, and meso-zeaxanthin. Meso-zeaxanthin is most highly concentrated in the epicenter of the macula, zeaxanthin in the mid-periphery, and lutein in the periphery of the retina.8 The macula's yellow color absorbs blue to UV light and behaves like protective sunglasses against damaging UV light.
Macular Degeneration (AMD, ARMD) is the gradual breakdown of the macula cells. Such deterioration weakens your ability to read, write, drive, and recognize faces. Peripheral, or side vision isn't damaged.
If there are any positives to macular degeneration, it is that, treated early-on, it is very responsive to nutritional support.
 Next: Nutritional support, diet, & lifestyle tips for macular degeneration.
Next: Nutritional support, diet, & lifestyle tips for macular degeneration.
Blindness is not inevitable for people who have ARMD. There is a large amount of peer review research showing ARMD to be a nutritional and lifestyle responsive eye disease, meaning that you can stabilize and possibly even improve your vision with healthy lifestyle choices.
You've probably received records from my 2/18 visit with my Ophthalmologist. Not only did the macula not degenerate at all, but my left eye seemed to be 20/20! Clearly it's your regimen and supplements that are making a huge difference! I'm so incredibly grateful!, K. N., Feb. 2020
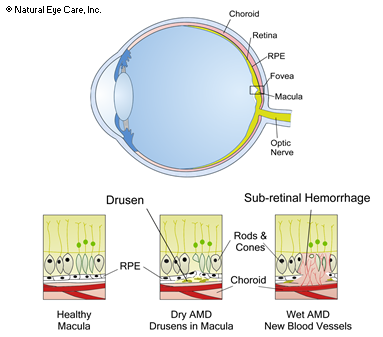
Most people with ARMD have dry macular degeneration. In dry macular degeneration tiny, yellow drusens develop. Drusens are accumulations of fatty, yellow material that form in the macula and people with ARMD have more and larger drusens than what is common with aging. They are thought to be comprised of waste proteins and lipids (oily material) that begin to accumulate due to poor circulation and waste-flushing in the eye.
In the absence of adequate antioxidants drusen slowly crowd, distort, or break the cells in the macula leading to deterioration and resulting in blurred vision. Because drusen also include immune-system regulating molecules, it is thought that they are part of the immune system.3
The second type of macular degeneration is the wet form, (also known as choroidal neovascularization) in which new blood vessels begin to develop near the macula, causing fast and serious vision loss. Wet macular degeneration can result from progression of dry macular degeneration, left untreated, and affects about 10% of macular degeneration patients.
If AMD is found first in one eye, the other eye follows the same progression. This is because the nutrient deficiencies and other system-wide problems would exist in both eyes but manifest in one eye before the other.
Pathology of Macular Degeneration
The development and progression of macular degeneration rests upon the occurrence of the following pathological changes in the eye.
- Oxidative stress - the imbalance between free radicals and protective antioxidants. The retina is especially vulnerable to stress from free radicals. Inability of the retina tissue to have enough oxygen available leads to deterioration of the pigmented layer which protects the retina from UV and blue light damage.5
- Angiogenesis - lack of oxygen leads to development of new extra blood vessels which distort the retina.5
- Apoptosis - cell death is a natural phenomenon in the body as worn and damaged tissue is removed and replaced. However in the retina excessive cell death is closely tied to oxidative stress.5
- Inflammation - the inflammatory response is the body's attempt to rescue tissue from cell injury. Proteins which are responsible for the immune results are among the constituents of drusen deposits in the retina as AMD develops.5
Symptoms
- Lines look distorted or wavy. (try the amsler test) In more developed AMD, the amsler grid can look quite distorted
- Shapes look blurred, fuzzy, or hazy in central vision
- Colors appear more dim and less distinct
- Words are hard to read because they are blurred
- Blank or dark areas hide the center area of your vision
- The center of vision looks foggy or cloudy
Causes

Other conditions
- Hypertension. People with high blood pressure are more likely to develop AMD than those with normal blood pressure.
- Diabetics are more at risk for AMD than others.
- Systemic inflammation, indicated by high levels of c-reactive protein has been tied to increased macular degeneration risk.2
- Diabetics are more at risk to develop AMD.
Biochemistry
- Free radicals can damage the eyes. They are formed when the blue and ultraviolet sunlight passes through the crystalline lens of the eye. Free radicals also result as natural metabolism byproducts. These chemical are highly reactive and cause oxidation. The result is destabilization of healthy macula cells in the eyes.
- High Homocysteine levels Studies have shown increased plasma homocysteine in patients with age-related macular degeneration.6, 7
Lifestyle/Diet
- Smoking, chronic fatigue and a weak immune system hasten damage from free radicals. Smoking increases the risk of AMD by 200-300%. In addition, there is a link between Alzheimer's disease and macular degeneration which is worsened by smoking.
- Poor digestion and nutritional deficiencies - People with ARMD are often deficient in a number of nutrients that are essential to eye health such as lutein, essential fatty acids, zeaxanthin, taurine, antioxidants, zinc, bioflavonoids, selenium, and vitamin B-complex.
- Low carotenoid levels. Read more about how carotenoids protect your vision.
Gender/heredity
- Heredity is a risk factor. People who have a family history of AMD are more at risk to develop the condition.
- Women are more at risk at developing AMD.
- Men who are obese have a higher risk than other men. This is associated with Western diets which are relatively high in fat and which contribute to a weak microbiota community in the digestive system. In addition to poor digestion not absorbing nutrients, this means higher levels of long-term, low-grade inflammation in the body which contributes to greater risk of macular degeneration.4
Drugs that can damage the retina
- Plaquenil (hydroxychloroquine sulfate), often prescribed for rheumatoid arthritis, has been found to cause permanent damage to the retinal.
- Chloridine (Catapres), for high blood pressure
- NSAIDS (non-steroidal, anti-inflammatory drugs) side effects from regular use include retinal hemorrhages. This group includes ibuprofen, aspirin1, ibuprofen, ketoprofen, flurbiprofen, and naproxen sodium. In addition acetaminophen (Tylenol), though not an NSAID, can harm vision.
- Also see a list of harmful drugs tied to macular degeneration.
About the Macula
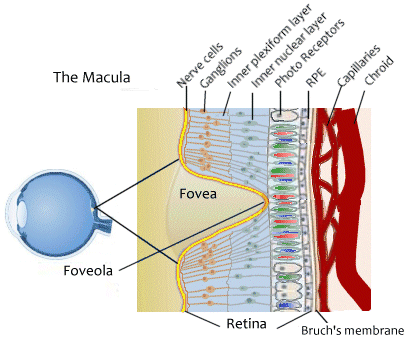
The macula contains two areas of unusually high concentrations of cones, which are the photoreceptors responsible for color vision, fine detail and central vision. There is a slightly depressed area in the center of the macula called the fovea where there are no retinal cells - only photoreceptors - about 199 to 300 thousand cones per square millimeter. At the center of the fovea is the foveola where there are only cones - no rods.
The gradual breakdown of the these cells in the macula results in damage to or loss of your central vision. The macula provides focus in the center of vision where your vision sharpness is most acute. Such deterioration reduces the ability to read and recognize faces, two important tasks that use the central vision.
AMD News
Want to learn more? See our blog news on ARMD and AMD.
 See
Vitamins & Supplements to support the retina and macula.
See
Vitamins & Supplements to support the retina and macula.
Related Conditions
- Poor circulation in the eye is a contributing factor to many eye conditions, and is a side effect of diabetes.
- Elevated homocysteine levels have been associated not only with macular degeneration but also glaucoma, diabetic retinopathy, optic neuropathy and ocular complications from Behcet disease.
- Choroidal neovascularization, also known as wet macular degeneration is the more advanced form of the condition.
- Macular pucker, or epiretinal membrane, in which a thin layer of tissue grows over the retina.
- Stargardt disease, is a form of macular degeneration affecting young people and caused by a gene mutation.
- Retinitis pigmentosa is a degenerative disorder of the photoreceptor cells of the retina.
- Myopic macular degeneration, also known as degenerative myopia, is characterized by severe elongation of the eyeball. Consequent tissue stretching and weakening can result in AMD-like changes at the back of the eye.
Research and Footnotes
See research on macular degeneration vitamins and supplements.
Footnotes
1. Liew G, et al. (2013). The Association of Aspirin Use With Age-Related Macular Degeneration. JAMA Int Med. Feb.
2. Mitta VP, et al. (2013). C-Reactive Protein and the Incidence of Macular Degeneration. JAMA Ophthalmol. 2013.
3. Hageman GS, et al. (2001). An integrated hypothesis that considers drusen ... macular degeneration. Prog Ret Eye Res. Nov.
4. Andriessen EM, Wilson AM, et al. (2016). Gut microbiota influences pathological angiogenesis in obesity-driven choroidal neovascularization.
EMBO Mol Med. Dec.
5. Pinazo-Duran MD, Gomez-Ulla F, et al. (2014). Do Nutritional Supplements Have a Role in Age Macular Degeneration Prevention? J Ophthalmol. Jan.
6. Coral K, Raman R, et al. (2006). Plasma homocysteine and total thiol content in patients with exudative age-related macular degeneration age-related
macular degeneration. Eye.
7. Axer-Siegel R, Bourla D, et al. (2004). Association of neovascular age-related macular degeneration and homocysteinemia. Am
J Ophthalmol.
8. Nolan JM, Meagher K, Kashani S, Beatty S. (2013). What is meso-zeaxanthin, and where does it come from? Eye (Lond). Aug;27(8):899–905.
Symptoms & Causes Vitamins & Supplements About the macula News
 info@naturaleyecare.com
info@naturaleyecare.com



 Home
Home


 Vision
Vision Vision
Vision



 Health
Health Health
Health Research/Services
Research/Services Pets
Pets About/Contact
About/Contact


