Macular Edema
Vitamins/supplements Symptoms Causes Self help summary News
Macular edema is swelling of the macula, the small area of the retina responsible for central vision, of which the central 5% of the retina is most critical to vision. The edema is caused by fluid leaking from retinal blood vessels into the macula. Blood leaks out of the weak vessel walls into a very small area of the macula which is rich in cones, the nerve endings that detect color and from which daytime vision depends. Blurring occurs in the middle or just to the side of the central visual field, it can appear like one is looking through cellophane. Visual loss may progress over a period of months, and can be very annoying because of the inability to focus clearly.
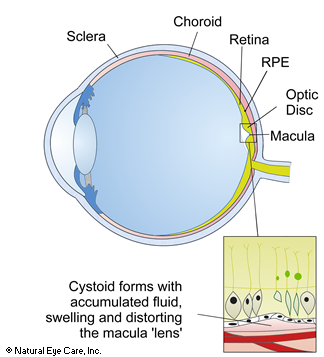
Because the macula is surrounded by many tiny capillaries, any conditions affecting the blood circulation anywhere in the body or in the eye can cause macular edema. Retinal capillary obstruction, inflammation of the eye, and age-related macular degeneration have all been associated with macular edema. The macula may also be affected by swelling following cataract surgery, but this normally resolves itself naturally.
ME rarely causes a permanent loss of vision, but the recovery is often a slow, gradual process over 2 to 15 months.
Symptoms
If you have these symptoms, your ophthalmologist can do a test called a fluorescein angiography or optical coherence tomography to accurately determine whether capillaries are leaking and if so, how severe the leakage is. These tests also measure how thick your retina is and the degree of swelling.
- Central vision seems blurry or fuzzy
- Vision is distorted, for example, straight lines may look wavy, especially when viewing the amsler grid
- Our vision seems pinkish looking
- We are more sensitive to bright light and glare.
Causes
Usually the cause is that tiny retina capillaries leak from weak vessel walls into the center of the macula. The patient perceives fogginess in the middle or just to the side of the central visual field, The loss of vision can occur slowly. It rarely causes an enduring loss of vision, but can take 2 to 15 months to heal. Sometimes macular swelling can occur after cataract or other surgery but is, with treatment, usually of temporary duration.
Because many tiny capillaries surround the macula, any condition affecting blood circulation in the body (diabetes, atherosclerosis, etc.) affects the eye; the result may be macular edema. The reason this is important is that macular edema is usually a symptom of a more serious health problem that needs to be addressed. In the case of the latter, macular edema typically occurs within 1-2 months post-surgery; though it can even happen many months, and even years, afterward.
Important. Anyone with diabetes should have their eyes checked annually, at the least, as there are a number of eye concerns linked to this disorder.
Here is a list of the possible key causes of macula edema:
- Oxidative stress. The imbalance between the antioxidant defense system, production of free radicals (reactive oxygen species, ROS), cause oxidative stress in the body and in the tissues of the eye. Damage from ROS causes a host of problems, including inflammation and fluid leakage in the macula and other parts of the eye.
- Other eye conditions. Macular edema is caused by many diseases, including optic neuritis, retinal vein occlusion, macular degeneration, diabetic macular leakage, eye inflammation, idiopathic central serous chorioretinopathy, anterior or posterior uveitis, pars planitis, retinitis pigmentosa, radiation retinopathy, posterior vitreous detachment, epiretinal membrane formation, idiopathic juxtafoveal retinal telangiectasia, capsulotomy or iridotomy. These disorders can be due to circulatory problems associated with hypertension, high cholesterol, etc.
- Other health conditions. The disorder can be related to general circulatory problems linked to hypertension, high cholesterol, and to nervous system-related conditions such as multiple sclerosis.
- Diabetes. A 2006 study of diabetics determined that 9% had macular edema; more recent evaluations find 3.8% in diabetics over 40. High levels of hemoglobin A1c, a biomarker for diabetes, are associated with higher diabetic macular edema risk. Having diabetes for 10 years or longer increases the risk.
- Medicines. A history of use of topical epinephrine or prostaglandin analogs for glaucoma is a factor.
- Eye surgery. Surgery for cataracts, glaucoma, or other retinal disease can result in macular edema, sometimes months after the surgery. Edema can occur due to post-operative lesions.
- Ethnicity. Non-Hispanic Blacks are at greater risk of developing diabetic macular edema.
- Injury. If you injure your eye and notice fuzziness in your central vision, be sure to see your eye doctor immediately.
- Inflammation. Inflammatory disease disorders such as cytomegalovirus infection, retinal necrosis, sarcoidosis, Behçet’s syndrome, toxoplasmosis, Eales’ disease, and Vogt-Koyanagi-Harada syndrome are often accompanied by macular edema.
- Drugs. History of use of topical epinephrine or prostaglandin drugs for glaucoma.
- Surgery. Cataract or other eye surgery
- Men are at higher risk
Conventional Treatment
The first line of treatment for macular edema is usually anti-inflammatory eyedrops. In certain cases, medication is injected into the back of the eye for a more concentrated effect, possibly along with an injection of steroids. Injections may include: Anti-VEGF (vascular endothelial growth factor) such as (Lucentis, Avestin, Regeneron, and/or Eylea). Steroids can also be implanted into the retina that slowly release medication overtime, including Ozurdex, Retisert, or Iluvien. Oral medications such as nonsteroidal anti-inflammatory drugs (NSAIDs) or steroids such as Prednisone may be prescribed to reduce the swelling.
In some cases, a vitrectomy may be recommended when blood has leaked in the vitreous (the gel that fills the area between the lens and the retina), due to pulling on the retina. This surgery is typically done on an outpatient basis.
Complementary Treatment
-
Get Vitamins & Supplements to Support the Macula
- Supplement your diet with a good multivitamin and/or a good green drink.
- Diabetics: If you have diabetes you are more at risk, prevention and early attention to symptoms will be valuable.
- Injury: Similarly, if you injure your eye and notice fuzziness in your central vision be sure to see your eye doctor.
- Healthy eye support recommendations These are very important for macular swelling.
Macular Edema News
Want to learn more? See our blog news on macular edema.
 info@naturaleyecare.com
info@naturaleyecare.com



 Home
Home



 Vision
Vision Vision
Vision



 Health
Health Health
Health Research/Services
Research/Services Pets
Pets About/Contact
About/Contact


